Leadership and Innovation Project, Essay Example
Introduction
Chronic obstructive pulmonary disease (COPD) is a disease characterized by limitation of airflow. It is also known as chronic obstructive lung disease (COLD), chronic obstructive respiratory disease (CORD), chronic obstructive airway disease (COAD), and chronic airflow limitation (Suzanne, 2000). Chronic obstructive pulmonary disease (COPD) is also a condition in which there is limited airflow in the lungs (Kerstjens, 2003). The disease develops and worsens over time, and although it is not reversible, its progress can be slowed with therapy.
Although COPD patients can normally breathe in well, changes in the small airways cause narrowing of walls during expiration therefore making it very hard to breathe out. The small sacs of COPD patients where oxygen and carbon dioxide are exchanged are destroyed and gradually starving the body of oxygen (Scott, 1961).
COPD is mainly associated with set of breathing-related symptoms:
- Being out of breath for some time when doing physical activities,
- Severe chronic cough
- Spitting and coughing mucus (phlegm)
The disease is also mainly due to co-occurrence of the chronic bronchitis as well as emphysema, which is a pair of commonly existing lung diseases in which the airways become narrow (Wilcken, 1962). This then leads to a limitation of the airflow to and from the lungs and therefore causing shortness of breath. In clinical practice, COPD is well defined by its characteristics of very low airflow on the lung function tests (Khoi, 1970). In contrast to asthma, this limitation is poorly reversible and it gets progressively worse over time (Jain, 1989). In England for an example, total estimated populations of 842,100 of 50 million people have a diagnosis of chronic obstructive pulmonary disease (Scott, 1961).
Chronic obstructive pulmonary disease is very common although it is preventable. In the recent years, it has led to great implications on health globally. Some Researchers have reported COPD as the third dangerous disease while others say it is the fourth most dangerous that leads to causing death (Kerstjens, 2003).
Chronic obstructive pulmonary disease is also a major cause of chronic morbidity as well as mortality over the world. Majority of people suffer so much from this deadly disease for many years and at long last die prematurely because of it and its complications. The Global Initiative for Chronic Obstructive Lung Disease (GOLD) has set up some goals for improving and preventing management of COPD through a worldwide effort to involve people in all aspects of health care as well as health care policy and at the same time encouraging a much expanded level of research towards this highly prevalent disease.
Terms of reference
This short project aims to explore the current issues and future issues as far as diagnosis, treatment, and management of COPD and other related ailment s is concerned. The project will borrow heavily from the available literature to deuce tangible conclusion and recommendations on the way forward in this aspect. It is my hope that the findings of this paper will be of utmost use to all stakeholders involved in the health sector.
Background information
COPD is a condition mainly caused by smoking and it is therefore preventable. It is a chronic condition that is very insidious, and which may not be diagnosed until it is fairly advanced with loss of about 50– 60% of lung functioning (Tandon, 1973). In the UK for an example, a total population of approximately 900 000 people have been diagnosed with COPD. However, the scale of this critical condition is probably underestimated, with as many as a further 450 000 people not diagnosed while others mistreated as to be asthmatic, which indicates that the prevalence of COPD may be much higher (Dorr, 1987). Majority of those affected are men compared to women, with prevalence rates being approximated at about 2% in men aged 45–65 years rising to 7% in men over 75 years (Bellamy and Booker, 2003). However, this trend is likely to rise in females over the next few years due to an increase of young girls in teenage age smoking.
The total annual cost of COPD to the National Health Service (NHS) has been estimated at over £980 million per year (Gibson, 2003). Half of this is due to inpatient hospitalization that results from exacerbation of symptoms. Costs that are within primary care are also high because it is estimated in primary care, an average GP with a list size of about 2000 patients will have 150 patients with COPD, therefore resulting in frequent surgery consultations as well as home visits. On average, patients suffering from COPD have two or three exacerbations per year and most likely treatment costs exceed far for those with asthma, mainly due to the high cost of oxygen therapy (Simon and George, 1990). Within secondary care, COPD patients account for about 10% of all medical admissions, therefore resulting in over 1000 admissions per year (Barnett, 2003) per average general district hospital. One important strategy to help in achieving the objectives of GOLD is by improving and providing health care authorities, health care staff, and the public with state-of-the-art data and information about COPD and its specific recommendations touching on the most important and appropriate control measures as well as management and prevention strategies. The major part of the GOLD report is mainly devoted to all clinical management of COPD and it presents a plan of management that has four main components: assessing and monitoring disease, reducing risk factors, managing stable COPD and managing exacerbations (Wilcken, 1999). GOLD is a partner organization in a program launched in March 2006 by the World Health Organization’s Global Alliance against Chronic Respiratory Diseases (GARD). Through the work of the GOLD as well as its cooperation with GARD strategies and initiatives, high progress towards better care for all patients with COPD will be highly achieved.
Chronic Obstructive Pulmonary Disease is also a deadly progressive illness characterized by airflow obstruction and dyspnea that afflicts over 12 million people and represents a leading cause of death in many countries worldwide (Singh, 1967). It is often associated with some kind of emotional distress as well as reduced psychosocial adjustment, which can result to physical functioning and at the same time impair quality of life negatively. However, some psychosocial consequences of COPD remain largely untreated for a long time (Corrin, 2003). A previous randomized research trial showed that coping skills training (CST) could improve pulmonary-specific quality of life among pulmonary patients awaiting lung transplant. To date, however, no studies have examined the effects of a caregiver-assisted CST intervention in patients with COPD with less severe disease.
COPD is caused by particles or gas, and most commonly from tobacco smoking, which then triggers an abnormal inflammatory response in the lung (Simon, 1990). The proper diagnosis of COPD requires lung function tests (Suzanne, 2000). The main important management strategies are cessation to smoking, vaccinations, drug therapy and rehabilitation, some patients opt to go for long-term oxygen therapy as well as also lung transplantation (Hansoti, 1960).
Worldwide, COPD ranked as the sixth leading cause of death in 1990, is now being projected to be the fourth leading cause of death worldwide by 2030 due to an increasing rates in smoking and demographic changes in several countries (Chabra, 2008). COPD is the third leading cause of death in the U.S. and the economic burden of COPD in the U.S.
Majority of nurses during their nursing careers have been largely involved in caring for patients suffering from COPD which is a major cause of morbidity and mortality (Kerstjens, 2003). Worldwide, COPD causes about three million deaths each year. In the UK in 1999, the number of deaths that were caused by COPD rose up to 32 155 (British Thoracic Society, 2002b), which translates to one in 20 of all deaths (Halpin, 2001), making it as the fifth leading cause of death (Social Trends, 1995). It is expected by the year 2020 COPD will be third in the rankings of the global impact of disease scale (Murray and Lopez, 1996). In Wales and England mortality appears to be greater in the urban areas, with particular strong association with poverty and lower social class and high smoking rates in this kind of group (Scott, 2007).
Literature review
PESTEL Analysis
PESTEL analysis is a business strategic planning tool that is employed to perform a thorough business macro environment analysis to determine the best decision to be made in any given instance so as to survive. It is a very useful business tool because businesses operate in constantly changing environment. In his review Philip Kotler, a Harvard professor, said that PESTEL is a vital strategic tool for measuring business potential, direction, growth or decline and current position. The acronym PESTEL stands for: Political, Economic, Social, Technological, Environmental and Legal forces. The COPD case can be analyzed using this method as follows:
Political
This has to do with politics of the day prevailing in a country. It is generally assumed that if political temperatures are down; businesses tend to flourish and the vice versa is also correct. In this particular case, it can be said that it is neutral and thus not expected to cause much rubble in the treatment and management of COPD. However, future political challenges can not be ruled out. For instance, the labor party wanted the sale of drugs related to this disease to be made available in all government health centers on a cost-sharing basis. Let us be optimistic that this little challenge will not continue into the future otherwise it will grow into a fully-fledged threat to patients of COPD (Kotler, 1998).
Economic
As already mentioned, the economic growth of UK has not been very good in the recent past, thus it is expected to pose a great challenge to the acquisition of necessary resources required in treatment and management of COPD. Unemployment levels, inflation, exchange rates and lending rates show disturbing trends. This may partly explain the reason why many patients die after leaving hospitals. Sadly, for this challenge, we have no control over it. Management can only mitigate for ways to cushion its operational costs from the effects of this economic meltdown.
Social
These are those social trends that are perceived to affect the business either in a positive or negative manner. They include such factors as age structure, demographics, rural-urban migration, literacy levels and cultural issues. In the UK majority of the population is ageing, this means that demand for health care will be increasing as time goes by. This is even made worse by the fact that COPD tends to be more prevalent among senior citizens than the younger generations.
Technological
These trends in new technology keep on advancing on daily basis. Technology can create new products and services as well as phase out existing ones. For instance mobile telephone created new business for GSM carriers whereas it spelled doom for other business like the postal and courier services. As far as treatment and management of COPD is concerned, there is growing evidence that in the future we will have more advanced equipment and drugs to treat and manage this disease. There are already ongoing researches over the same in different parts of the world (Adams & Hendershot, 1996).
Environmental
These include such factors as climate and weather changes in a period of time. Changes in environment are hard to determine or control and they have greater impact on businesses either directly or indirectly. For instance if there is a drought, farming will be affected directly and this will also have an impact on people leaving with COPD. The deteriorating state of the environment mans that more and more people will become patients of this disease whereas those already affected will find it hard to recover. Issues like air pollution and its effect on COPD patients have become very disturbing among the medical personnel. Sadly, there is little that management of medical services can do to change this scenario.
SWOT Analysis
SWOT analysis is a very popular business tool that is used to analyze internal environment of a business concern. This is a strategic planning method that was developed by Albert Humphrey in the 1960s. It is a very popular tool for measuring business projects viability before making any serious investments. The acronym SWOT stands for Strengths, Weakness, Opportunities and Threats. Strengths and weakness are internal to the firm and deal with those factors that are seen as either advantageous or otherwise to the business in carrying out its operations. The business has a complete control over it and can therefore change to its own success. On the other hand opportunities and threats are those factors that are either advantageous or disadvantageous towards a firm’s operations from external point. Since they are external to the business, the firm has little control over them. It can only devise strategies to deal with them (Kotler, 1998).
Strengths
These are the factors available within the firm that that give the firm an edge over the rest of the firms in the same industry. In these particular case strengths that have been identified include availability of equipment, skills and knowledge necessary in handling OCPD. These strengths need to be tapped fully. Others are good interpersonal relation skills, team work among the nurses and availability of smoking cessation skills.
Weakness
These are those factors that are available within the firm that work against it. If they outweigh the strengths, you are bound to fail. In this particular case, the weaknesses identified include inadequate number of staff, reactive staff and lack of pro activity in screening COPD patients. These can be easily addressed by management to the benefit of patients with COPD.
Opportunities
These factors pose potential benefits to the organization if they are well utilized. They only need to be identified and exploited. To begin with there seems to be increased lung health among population coupled with increase in COPD list size. This means in the future we are likely to have a health population thus release more stress on the already overstretched facilities in hospitals. Other opportunities available include developing staff, teamwork improvements and influencing of local policies for our own benefit.
Threats
These factors pose possible dangers to the organization. They need to be identified and corrected well in time before they bring about serious challenges to the organization. Threats that have been identified in this scenario include increased workload, unwillingness of patients to come for early screening. This poses serious threats to the management and treatment of COPD. Other threats also include time and other related constraints. This also hampers the advancement of treatment to COPD patients.
Epidemiology
COPD is characterized by obstruction of airflow and other breathing related symptoms like
Expectoration, exertional dyspnea, chronic coughs and wheezes. It has been categorized with
Air flow limitations. Airflow limitation is associated with an abnormal response of lungs due to inflation of gases. This is due to combination parenchyma and airway damage. Obstruction of
Airflow is defined as the reduced post-bronchodilator FVC /FEV1 ratio (where FEV1 is forced
Expiratory volume in 1 second and FVC is forced vital capacity), such that FVC /FEV1 is less
than 0.8. If FEV1 is 79% or more of predicted normal, COPD diagnosis should only be made during the presence of respiratory symptoms, e.g. cough or lack of breath (Rennard, 1998). PaCO2 normally initiates the respiratory drive but in COPD the strongest driving force is hypoxia. This means that COPD can be reduced if hypoxia is controlled. Normally, patients with COPD have been categorized in two, blue boaters and pink puffs.
- Blue bloaters are blue because of polycythamia and hypoxia. The often have water retention and they are obese. They depend on hypoxia for their respiratory drive and provision of oxygen, which insufficient of it will lead to significant hypercapnia, and imbalance of the acid base.
- Pink puffers are those who have a problem of maintaining pO2. The common symptom is barrel-shaped hyper inflated chest and use pursed lips for breathing.
The damage to the lungs is caused by chronic inflammation, caused by smoking tobacco. Other factors like occupational exposure may also be a big contributor of chronic obstructive pulmonary disease development. According to a study conducted in the UK, three million people are estimated to be suffering from COPD and about 900,000 have been diagnosed with it. Other two million people are yet been diagnosed with COPD (Hansen & Phanareth, 1999).
COPD rate in the population is estimated to be between 2% and 4% with a diagnosed prevalence of 1.5%. Prevalence increases with age with an estimation of 10% prevalence in men older than 75 years. Mostly patients diagnosed only when the attain fifty years. Levels of deprivation highly influence the rates of COPD in that communities that are more deprived have higher rate of COPD.
Previous studies
Depression is the main cause of most Chronic co morbidities. Previous studies have been conducted to explore the association between depression and COPD. A large population based study was conducted to determine the risk of developing a depression diagnosis in association with the previous diagnosis of COPD (Enright and Johnson, 1991).
The General Practice Research Database in the UK was used to assess and compare the prevalence of depression history and likewise measure the risk of developing an incident depression for patients suffering from COPD and those that are not affected between1995 to 2005. A nested case control analysis was conducted, matching up to five patients who showed symptoms of developing depression for each case who did not develop depression. This was done to analyze the impact of COPD severity.
The results showed that, in a population of 35721 patients suffering from COPD and 35771 without COPD, the prevalence of diagnosed depression compared to the first COPD diagnosis was much more in the population with COPD (24.1%) than among patients who suffered from COPD (17.8%) The rate of incidence of a new diagnosis of depression after the previous COPD diagnosis was 17.2/1,000 person-years (py) of the COPD group, whereas it was only 10.4/1,000 py in the COPD free comparison group. In this case, control analysis, the patients with severe COPD had a higher risk of developing depression (odds ratio, 3.01; 95% CI, and 2.45–3.78). A conclusion based on the large study was made that COPD patients are in an increased risk of developing depression (Enright &Johnson, 1991).
Legislative framework
As from 2005, the NHS, patients, clinicians and the department of health have worked jointly towards the establishment of the best ways of improving care for patients of chronic obstructive disease (COPD) and the reduction of the amount of people with the disease. They aim to come up with a strategy that will ensure that all the patients who are diagnosed with COPD have access to responsive, equitable, high quality and better provision of social and health care services from the right people at the right place and at the right time. These services should be cost effective hence provide good value for taxpayer’s money (Pauwels and Buist, 2001).
To advise how the local communities will prevent people from contacting COPD, secure diagnosis improvement, understand risks of poor lung health, offer care to patients of COPD and reduction of health inequalities. It should also support patients of COPD and those who take care for them with practical education, advice on how to manage the disease.
The strategy aims at providing advice and support for hospitals, commissioners, general practice, strategic health authorities and primary care trusts (PCT). These components of NHS should deliver services for COPD while developing, planning and monitoring services (Pauwels and Buist, 2001).
Another huge health problem in England is Asthma. COPD’s national strategy will contain sections that will highlight there is a common area of approach of these two diseases and where there is a difference. Good asthma services have also been highlighted.
Clinical governance and risk management
A clinical governance arrangement needs to be developed to allow the safe and effective management of a complex network of COPD care. Clinical governance performance by multidisciplinary teams will require practices and structures that encourage the NHS and other relevant bodies to engage in conversions that are focused on detailed composition of COPD care. According to Respir (1995), these conversions should deal with questions like:
- Is COPD being addressed properly? Given the assessed health needs and the resources constraints that exist. In addition, is the value for money being delivered? For COPD, how effective and appropriate are the services offered.
- The management of clinical performance for COPD according to the national codes of clinical practices should be top notch. COPD care should be systematized and performed with safety, risk, quality, patient evaluation and with an aim of attaining positive clinical outcomes.
- Treatment should keep up with the latest developments and done to the extent of the best capability and strategies should be put into place for professional development and service to COPD patients treatment. There should be staff appraisal and review, clinical mentoring and leadership development.
To enable these conversions we require actions at the level of organizational structure as well as clinical practice. The practice level requires implementation and development of integrated care pathways for COPD.
Risk assessment, including organisation, leadership and an informed picture of the possible hotspots for change management, the resisting and driving forces, based on the reality of the people involved and the managerial and local clinical policies (Respir, 1995).
Ethical issues
Acute exacerbations are frequently experienced by those patients with severe airflow obstruction. This can cause failure of the respiratory system and possibly ventilation support should be availed. The hospitalization of this disorder identifies a group of COPD patients with guarded long term prognosis. Among this type of patients, 90% survive to discharge from hospital. Survival to discharge reduces to 75% when intubation with mechanical ventilation is required. Only 58% of such patients remain alive one year after discharge with poor quality of life caused by unremitting respiratory symptoms (Rennard, 1998).
Additionally Rennard (1998) maintains that the guarded prognosis poses an ethical issue of patients with COPD who may not get sufficient help from mechanical ventilation and intubation if their disease is more advanced. This may result to poor quality of life and a minimal possibility of recovering from ventilator support. Unfortunately, there are no clinical factors that can accurately identify those patients who might not benefit from life supportive care at the time of hospital admission. Without accurate prediction of clinical outcome, the caregivers have to address and recognize the ethical issues that may arise in caring for patients with the advanced COPD.
Human rights
These are rights that should be enjoyed by COPD patients during care, treatment and management of COPD. They are embedded in the constitution and hence any body found violating them is liable to face prosecution in a court of law. This means in our endeavors to deliver services we should do our best to act within the provisions and limitations of the law. According to Pauwels and Buist (2001), these rights are as follows:
- Right to receive accurate and early diagnosis. Early and accurate diagnosis is vital for COPD patients to allow them to take necessary precautions towards improving lung health and quality of life.
- The right for education and information about COPD. Is important to for people in each country to what COPD is, what the major causes are and what its symptoms are.
- The right for understanding and support. Family, communities, health care providers, friends and health services need to offer understanding and support to COPD patients.
- The right to investment in their welfare and care as well as their fair share of involvement in the society. Patients of COPD have been working throughout their lives towards earning their fair share of involvement to the society.
- The right to receiving treatment and care that will help them. Proper treatment and care will be beneficial to patients by improving their quality of life, breathing and will help them to contribute more to others.
- The right to conducive environment and safe air. Unsafe environment and air are harmful to COPD patients. It is an obligation of all health care professionals to protect the patients from unsafe conditions.
- The right of advocating with other COPD patients and supporters for improved COPD prevention and care. COPD patients know that good care is very important to them. They also recognize that efforts should be made to prevent others from contacting the disease. It is therefore their right to advocate for improved COPD prevention and care.
Change management
Resistance to change is one of the biggest barriers that organizations face in their endeavor to implement change. This greatly hampers the uptake of new technologies, new ways of doing work and even progress of organizations. Reviewing on this, Osborne and Brown (2005) noted the following as some of the reasons that have been advanced as to why individuals may resist change.
- Feeling that management or colleagues are not competent enough
- Loss of control or authority that they have been enjoying
- Belief that change initiative is a temporary fad
- Lack of faith in themselves
- Loss of social standing
- Feeling that job security may be lost
Therefore, if I am the one responsible to bring change in an organization, the starting point will be to identify and anticipate reasons as to why workers may be against a particular organizational change. It is only by identifying some of the challenges that I can come up with practical and workable solutions. One sure way of handling a problem is to know what causes it in the first place.
More over Ferlie, Lynn and Pollitt (2005) goes further to cite the following as some of the signs that employees are not ready to change. This includes total failure, half-hearted efforts to change, sabotage of management’s efforts or even intentionally breaking down the systems. It is important to note that some individuals resist change due to multiple of reasons. Nevertheless, to mention I shall not take at face value the individuals stated reasons of resisting to change. This is because sometimes the stated reasons hide the real underlying reasons. Individuals work through a psychological change process as they give up the old and embrace or still reject the new.
Individuals may experience an initial denial, and then start to realize that the change is inevitable. Strong feelings may emerge e.g. frustration, anger, fear and helplessness. At last the person may accept change either negatively, with feelings of resignation or positively with renewed enthusiasm to capitalize on the changes. In the meantime, I will take note of those individuals who are stuck in one point. Offer them my support and give them room to work through the stages. I will give them time to breath and listen to them genuinely with empathy.
Leadership style
To be able to bring about change in this scenario, you need to look identify for a good style that can easily bring about the desusred change without much resistance. After a careful study and consideration of all the available leadership styles, I settled for Democratic leadership style. This is the most popular leadership style of the 21st century. Its application in business circles, government ministries’, political set ups etc cannot be over emphasized. Democratic style remains the most popular leadership style due to the positive reaction employees have towards it. It entails seeking other peoples opinion over the decisions that are deemed to affect them. Followers prefer this approach because their self interests attracts them towards the leader besides giving them confidence over their actions.
Conclusions and Recommendations
Conclusions
COPD is a very challenging disease to both treat and manage. There is need for all stakeholders involved to work together to help the people affected by this disease from further suffering. Doctors, nurses, government, researchers and even patients themselves should improve the way they handle this disease to stop the situation from getting worse.
The following Gant Chart summarizes the time line of the various activities in this project.
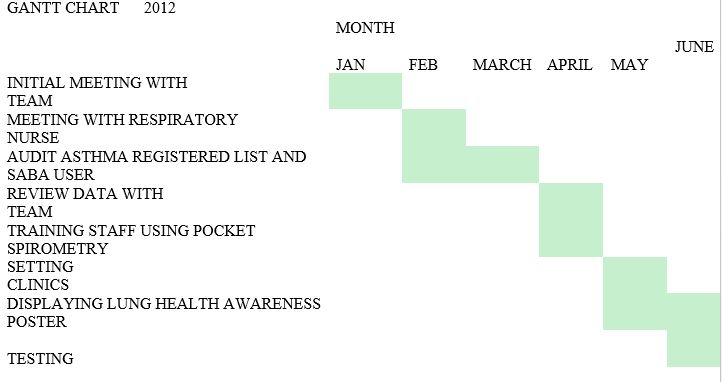
Recommendations
- There is need to come up with new laws and legislations governing the diagnosis, treatment and management of COPD.
- There is a need to establish specialized hospitals to deal with patients suffering from COPD so as to give them more specialized treatment and stop the probability of infecting others
- The old saying that prevention is better than cure should be encouraged so as to stop new infections from taking place. For instance, this can be achieved by increased awareness campaigns on how one can protect him/herself from contracting COPD.
References
Osborne SP and Brown, K. 2005 Managing Change and Innovation in Public Service Organisations London: Routledge.
Ferlie, E, Lynn, L and Pollitt C. 2005, The oxford handbook of public management. London, Oxford University Press.
Suzanne H, 2000. The impact of COPD on drug health worldwide, epidemiology and incidence. Chest journal
Simon George, 1990 High density shadows & hypertransradiances, Gold report
Butterworths & Jaypee brothers, 1990. Principles of chest X-ray diagnosis, 4th edition. New Delhi Postma S D & Kerstjens A, 2003.Epidemiology and natural history of chronic obstructive pulmonary disease.
Gibson G J, Geddes M D, Costabel U, Sterk J P & Corrin B, 2003. Respiratory Medicine. 3rd ed.
Saunders Wig KL Guleria JS, Bhasin RC, Holmes JR. E, Vasudeva YL and Singh H, 1967 Certain clinical and epidemiological aspects of chronic bronchitis as seen in Northern India. Indian Chest Disorder
Tandon MK. 1973, Correlation of electrocardiographic features with airway obstruction in chronic bronchitis. Chest
Singh VK & Jain SK. 1989, Effects of airflow limitation on the electrocardiogram in chronic obstructive pulmonary disease (COPD). Indian Journal Chest
Spodick D, Kelvene J, Tyler J, Muesch H & Dorr C, 1987 The electrocardiogram in pulmonary emphysema. Relationship of characteristic electrocardiographic findings to severity of disease as measured by degree of airway obstruction. Am Rev Resp Dis.
Carid FI, Wilcken D, 1962, In chronic bronchitis with generalised obstructive lung diseases – Its relation to ventilatory junction. Am J Card.
Scott RC, Kaplan S, Fowler O, Helm RA, Westcott RN & Walker IC, 1955. The electrocardiographic pattern of right ventricular hypertrophy in chronic corpulmonale Circulation. Pinto, Hansoti R, 1960, The ECG changes in chronic corpulmonale. J Assoc Phy India.
Calatayud JB, Abad JM, Khoi N, 1970, P-wave changes in chronic obstructive pulmonary disease. Amer Heart Journal.
Scott RC, 1961, The electrocardiogram in pulmonary emphysema and chronic corpulmonale. Amer Heart Journal.
Rich Stuart & McLaughlin V, 1835, Pulmonary hypertension. Chapter 67. In: Braunwald’s Heart Disease, 7th edition. Elsevier Saunders
Harold M. Silver , Juan B. Calatayud, 1971, Evaluation of QRS Criteria in Patients with Chronic Obstructive Pulmonary Disease. Chest
Thompson H, North L & Aboumrad M,1973, Electrocardiogram in chronic obstructive pulmonary disease. Amer Rev Resp Disease
Ruskin J, Estes E Jr & Greenfield J,1969,The electrocardiogram in chronic obstructive lung disease. Southern Med Journal
Burrows B, Niden A & Barclay W, 1965, Clinical and physiological findings in 175 patients and their relationship to age and sex. Amer RevResp Dis
Agarwal R, Dinesh Kumar, Gurpreet, Agarwal D & Chabra G, 2008, Diagnostic Values of Electrocardiogram in Chronic Obstructive Pulmonary Disease (COPD), Lung India.
Rennard S,1998. COPD: overview of definitions, epidemiology, and factors influencing its development . NY. US
Benson V& Marano M, 1995. Current estimates from the National Health Interview Survey Vital Health
Mannino M & Gagnon R1994, Obstructive lung disease and low lung function in adults in the United States: data from the N H and N ES. USA
Respir C, 1995.Standards for the diagnosis and care of patients with chronic obstructive pulmonary disease. AmericanThoracic Society
Siafakas N & Vermeire P, 1995. Optimal assessment and management of chronic obstructive pulmonarydisease. The European Respirator Society Task Force.
Pauwels R & Buist A, 2001. Global Strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. NHLBI/WHO
Dirksen A & Christensen H, 1991,. Bronchodilator and corticosteroid reversibility in ambulatory patients with airways obstruction. Dan Med Bull.
Bestall C & Paul E, 1999. dyspnoea scale as a measure of disability in patients with chronic Obstructive pulmonary disease. Medical Research Council.
Adams P & Hendershot G, 1996. Current estimates from the National Health Interview Survey, National Center for Health Statistics.
Kanner R & Connett E, 1994. Gender difference in airway hyper responsiveness in smokers With mild COPD. The Lung Health Study.
Enright P & Johnson R,1991, Spirometry in the Lung Health Study. Methods and quality control. UK.
Chang J & Moran M, 1995, COPD in the elderly. A reversible cause of functional impairment. Tokyo, Japan
Hansen E & Phanareth K, 1999. Reversible and irreversible airflow obstruction as predictor of Overall mortality in asthma and chronic obstructive pulmonary disease. Jersey. USA
Ulrik C & Backer V,1999. Nonreversible airflow obstruction in Life-long nonsmokers with moderate to severe asthma. Eur Respir
Kotler Philip (1998). “Marketing Management – Analysis, planning, Implementation, and Control”, 9th Edition, Englewood Cliffs: Prentice-Hall.

Time is precious
don’t waste it!

Plagiarism-free
guarantee

Privacy
guarantee

Secure
checkout

Money back
guarantee






